The health insurance industry is undergoing profound structural changes that will affect employers -- and you must be ready to capitalize on these changes.
Most notably, health insurers are moving away from the “fee for service” reimbursement system whereby health provider networks are paid a negotiated (reduced) fee for services. Or put simply: the more services a health provider delivered, the more it is paid.
This fee-for-service model costs employers dearly, largely because providers and patients tend to overuse the healthcare system. What’s worse is that fee-for-service largely delivers inadequate care and unacceptable outcomes. As a result (according to my estimation as the CEO of a health insurer), this has led to employers paying over 30% to 40% more for health insurance coverage.
According to Michael Porter of Harvard Business School, the solution lies in healthcare outcomes. “The overarching goal for providers, as well as for every other stakeholder, must be improving value for patients,” says Porter in The Strategy That will Fix Health Care (Porter & Lee, Harvard Business Review, October 2013). “Value is defined as the health outcomes achieved that matter to patients relative to the cost of achieving those outcomes.”
Fortunately, the nation’s healthcare system is moving toward a different payment paradigm. These changes provide opportunities for employers to redesign their insurance benefit packages and prepare employees for significant changes ahead.
If done correctly, employers can reduce claims costs spending and have healthier employees. But to achieve these benefits, employers can’t sit on the sidelines and take whatever is offered by insurance carriers.
Five Steps to Redesigning Company Health Insurance Benefit Packages
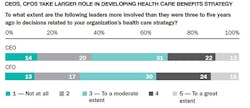
1. Move Health Care Into the C-Suite
Most companies have traditionally left health care coverage and premium negotiations to HR departments and insurance brokers. No more. Going forward, employers must move beyond insurer account reps and demand access to insurers’ senior management for frank discussions on whether the insurer is willing to proceed down this path.
Your senior management (i.e., the CEO) should be present at the first meeting to ensure you get access to the insurer’s senior management. Believe me, it makes a difference, which I observed firsthand as CEO of a health insurer. These types of meetings had an impact on me and attending staff. If the insurer is not willing to proceed in this direction, and assuming you have the option, it’s time search elsewhere. Let them know this.
2. Negotiate New Business Designs
Right now, employers should schedule an initial meeting with insurers to discuss how they are redesigning insurance plans to motivate providers around quality of care, better outcomes, and reduced expenses rather than increasing quantity.
All signs point to a change from fee for service reimbursement to bundled payments--plus, a methodology that shifts some financial risk from insurers to providers who then manage their assigned populations to avoid financial loss due to excess services. This will incent providers to provide needed care and no more.
The ultimate goal is moving away from zero-sum negotiations toward aligned partnerships amongst employers, employees, insurers and ACOs...
Also in the near future, ACOs will receive additional payments based on superior care and outcomes. This is the “plus,” and it will incentivize better care and better outcomes. For employers who pay the premiums, it means far more value for the dollar spent, and over time, a reduced spend.
The ultimate goal is moving away from zero-sum negotiations toward aligned partnerships amongst employers, employees, insurers and ACOs that advance the common goal of better care, better outcomes, and reduced costs so that employers can maintain quality coverage for their employees.
3. Demand Transparency
Today, we shop blind. There is no effective way to determine which physicians or providers deliver high quality, better outcome, lower cost care. This lack of information affects primary care physicians’ ability to make informed referrals or know where the rate falls on the quality and outcomes spectrum.
Similarly, it’s nearly impossible to learn the cost of many healthcare services. Yes, we can determine the cost of an office visit, but what about a multi-disciplinary procedure like open heart surgery? Lack of price transparency not only affects employees’ ability to choose the best, most cost-effective providers, it hurts employers that spend premium dollars without any way measuring received value.
“Employers must demand that insurers make healthcare price, quality and outcome information easily accessible for employers, employees, and physicians on their websites and by telephone.”
Employers must demand that insurers make healthcare price, quality and outcome information easily accessible for employers, employees, and physicians on their websites and by telephone. For example, for an open heart surgery procedure, insurers should provide price and quality/outcome measures on all hospitals providing such services within 100 miles.
This is a marketplace issue and customers (i.e., you the employer) have leverage. The more employers demand these changes, the more providers and insurers will promulgate agreed upon measures of quality of care and outcomes. As CEO of Blue Cross Rhode Island, I met with the CEOs of insured companies. Believe me, if they challenged me on issues, I listened and assigned responsibilities to key management to address their concerns.
Once measures are in place and provider scorecards made available, insurers must base reimbursement on these measures. Physicians and hospitals should earn acceptable scores before insurers include them in their networks. Benefit designs (deductibles and copayments) should also be based on scores (i.e. high scores result in no deductibles; low scores result in large deductibles).
4. Focus on Outcomes
In my estimation, in 3 to 5 years healthcare providers will be highly incented to obtain superior outcomes and efficient, cost-effective, better quality care. Why are outcomes more important than quality of care? Because that is what’s most important patients and competitive alignment will help employers enjoy better value for their premium dollars.
As insurers use newly transparent data to drive results through benefit designs, networks, and changed reimbursement, employers will see a huge behavioral change amongst physicians and hospitals as they focus on quality and outcomes which should moderate costs. Once we cross that divide, employers will be armed with metrics that can be shopped around.
5. Develop Insurer/Primary Care Relationships
Healthcare costs will remain an issue if employees do not take better care of themselves and access the healthcare system more responsibly. Inappropriate emergency room visits, non-compliant diabetics, untreated obesity, and untreated or undiagnosed mental illness such as depression are types of factors that cost employers easily a third of their healthcare spend.
The solution is improving patient compliance, a task that must be shared by insurers, primary care physicians, employees and employers.
When employers obtain this type of cooperation, they can achieve extraordinary savings ranging from reduced waste, reduced medical error, fewer self inflicted illnesses, and less misuse of the system.
A Personal Case Study in Redesigning Health Insurance Benefits
While I served as CEO of Blue Cross & Blue Shield of RI, we made significant strides in rethinking primary care by creating patient-centered medical homes, which dramatically improved overall patient compliance, among other things. This approach helped patients meet office visit requirements, improve prescription drug compliance and lower patients’ overall blood-pressure and weight-loss numbers.
This program was successful because part of what we paid providers was based on results. Physicians were no longer driven to maximize their daily number of patients. We dramatically reduced emergency room visits by incenting the patient-centered medical home to be open evenings and on weekends, and by the physicians and nurses educating their patients about why using the patient-centered medical home rather than the ER made sense. Though office visits increased due to our focus on preventive care, we made huge savings on more serious illnesses or hospitalizations.
Employers must demand that insurers develop new plans that incent patient compliance in new and innovative ways. Insurers can avoid confidentiality constraints, given that insurers have access to patient health records enabling them to create individualized plans. Patient compliance is where insurers can differentiate themselves from competitors in the new world of healthcare, but that differentiation must be measurable and provable.
First, employers should be clear about program parameters. For example, how intrusive will the interventions be with your employees? What types of interventions will you want? What about union concerns? You must make a specific ask of your insurer, which means doing your homework.
Next, employers must initiate candid meetings with insurers to address several key questions. Is your request doable? Can the insurer identify anything you may have overlooked? Is the insurer working on this now and when will it be implemented? Will the insurer invest in patient compliance and measurable outcomes, and what might this look like? Where is your insurer vis a vis primary care and patient centered medical homes (a principal driver of patient compliance under any scenario)?
Finally, make it clear to the insurer that without a meaningful patient compliance program based on a timetable with deliverables, they risk losing your business. Ideally, your insurer is already moving in this direction and your meeting may accelerate this movement, particularly if other businesses do the same.
Addressing the Challenges of Redesigning Insurance Health Care Benefits
Changing a decades old model will not happen overnight. This strategy will require at least three years to fully develop. However, it really is the only alternative to throwing premium dollars down the drain and continuing the zero-sum game of employees of paying more and paying increasing deductibles, reducing coverage or getting out altogether.
There is strength in numbers. Although it’s unlikely that insurers will tailor a program for one employer with less than 2,000 employees. Smaller companies should consider joining forces with similarly situated companies via associations or collaboratives.
Many underwriting rules prohibit companies from banding together solely for the purpose of purchasing health insurance. But Chambers of Commerce and trade organizations can organize and negotiate on behalf of their members. Now’s the time to explore these options with appropriate legal and healthcare professionals.
Five years ago, this approach would have been laughed at. This is no laughing matter today, and in my opinion, it is the only viable route to higher quality care at appropriate prices.