As They Help with COVID-19 Relief Efforts, Automakers Tackle Their Own Safety Issues
In the past few weeks, automakers in the United States and Canada have made headlines for their willingness to step up and produce ventilators and masks as hospitals deal with a severe shortage of equipment for the onslaught of coronavirus patients already arriving at their doors.
But how can they mobilize to make complex devices like ventilators, which can have over 600 individual parts that need to be sourced, all the while dealing with their own issues around the virus and keeping their workers safe?
Julie Fream, president and CEO of the Original Equipment Suppliers Association and Colin Dhillon, CTO of the OESA’s counterpart in Canada—the Automotive Parts Manufacturers’ Association—offered a glimpse into the questions automotive suppliers and OEMs are trying to answer around the crisis and how they can help. They made their comments in a live April 3 webinar moderated by Carla Bailo, president and CEO of the Center for Automotive Research, the independent automotive research non-profit based in Ann Arbor, Michigan
Automotive OEMs have purchasing power to contribute and the ability to manufacture in large quantities and improve efficiency on large production lines that haven’t had that demand, said Fream. The OESA’s members are “lending their expertise to help with things like lean manufacturing” to ramp up ventilator and Personal Protective Equipment (PPE) production.
Last week, Canadian Tier 1 suppliers Magna, Linamar, Martinrea and ABC Technologies announced they would work as a support team helping medical device companies produce 10,000 ventilators paid for by the province of Ontario.
Ten thousand is only a fraction of what the country needs, said Dhillon, but he expects the Canadian government to soon make announcements about additional partnerships. Canada currently has 5,000 ventilators and will need an estimated 80,000 to 100,000 ventilators if the trajectory doesn’t flatten.
Fream called out the “hidden heroes”—smaller Tier 2 and Tier 3 automotive suppliers that are stepping up to produce many of the ventilator components.
“GM has talked about [manufacturing] ventilators, and it’s over 600 individual components, and they were able to source those over the course of 48 hours,” she said. “It may just be a bearing or small plastic part, but we all have to come together.”
Likewise, automotive manufacturers like Ford and GM making ventilators in-house must rely on expertise from medical-device partners, said Dhillon. “Unless you’ve got some of that medical manufacturing background, you are really going to be starting from scratch and the ramp-up could be weeks, months,” he said. APMA is working with McMaster University in Hamilton, Ontario, and building a consortium with technical and medical OEM experts to work on “something like the Medtronic open-source ventilator.”
Fream said that OESA is working with the U.S. Federal Emergency Management Agency (FEMA) to understand the extent of demand for ventilators as the crisis progresses, and how best to deploy manufacturers “that can do this and can support it.” That may mean subcontracting the work from the existing medical device and PPE manufacturers and working within their existing designs and technology.
The OESA is also working with the National Manufacturers Association to survey members and get a better understanding of what the capacities and capabilities are within industry, “and getting that information to FEMA so they can begin to source” and avoid duplication of efforts.
In Canada, part of the APMA’s legwork involves collecting federal government and Health Canada specifications for all the different types of equipment needed. “For instance, face shields don’t necessarily have to be manufactured in a clean room, but a face shield must be worn by all of those assembling the components,” Dhillon said. “Where a mask may require a clean room.”
The costs involved are a concern, especially in the long-term, but at this stage, “there’s a true feel-good factor in this,” said Fream. “There’s a pulling together of the workforce behind this and the team of people supporting this.”
Meanwhile, auto industry manufacturers large and small are creating a whole new playbook for keeping their workers safe as the virus rages through communities. For instance, most OEM automotive production is shut down temporarily, but “what are our plans for when the OEMs all go back, and then the supply chain goes back to work?” wondered Dhillon. “At a Tier 1 supply chain facility, if an employee tests positive for COVID, what does that 500-employee manufacturing facility do? Do they send all 500 home or send only those people that are associated with the individual and maybe the cell the employee worked in? Question mark, question mark, question mark.”
Technology may be an answer—one possibility is location-tracking employees with a random ID number tied to their cellphones to identify who to quarantine in a plant—but of course there are privacy concerns, said Dhillon.
Fream said to expect many things to permanently change around the manufacturing workplace as a result of the coronavirus. “Healthcare is going to change, health insurance,” she said. “In terms of the manufacturing facility—touchless doors, touchless water fountains … Some manufacturing lines are being modified to allow for social distancing, or creating barriers between workers where they cannot create an appropriate social distance. I see lunchrooms and canteens being reorganized. There’s a whole set of new cleaning standards that need to be implemented—hourly, daily as well as a deep clean should you have an outbreak.”
Some plants are taking employees’ temperatures as they enter the building. Some are creating zones and staggering start times, “so that you have distinct areas of employees that don’t cross and intermingle with each other,” said Fream.
There are also new innovation possibilities with new partnerships, “just as thermoforming came out of building canopies for the Spitfire [fighter aircraft] in the U.K. back in the 1930s, early 1940s,” said Dhillon. “How do we take the autonomous technology, IoT technology and build maybe bots, or smart doorframes which are providing a mist and desanitizing us? Or why does an individual have to come up and put a thermometer on your head when a robot could do this and provide kits and sanitizing gels? I would like to see how we take the bot side, the autonomous side and really help to provide some safety.”
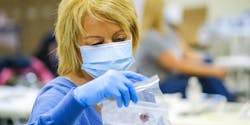
Main Photo: A General Motors employee reports to her first day of work making ventilators at GM's Kokomo, Indiana, plant. Employees started work on the ventilators on March 31, in partnership with Ventec Life Systems.
About the Author

Laura Putre
Senior Editor, IndustryWeek
As senior editor, Laura Putre works with IndustryWeek's editorial contributors and reports on leadership and the automotive industry as they relate to manufacturing. She joined IndustryWeek in 2015 as a staff writer covering workforce issues.
Prior to IndustryWeek, Laura reported on the healthcare industry and covered local news. She was the editor of the Chicago Journal and a staff writer for Cleveland Scene. Her national bylines include The Guardian, Slate, Pacific-Standard and The Root.
Laura was a National Press Foundation fellow in 2022.
Got a story idea? Reach out to Laura at [email protected]